Signed in as:
filler@godaddy.com
Signed in as:
filler@godaddy.com
If you have a large number of moles, a history of melanoma or have a family history of skin cancer, you may benefit from skin cancer surveillance. This involves you attending on a regular basis either 3 monthly, 6 monthly or yearly for a full skin check.
Dr Aaron Wernham is a Consultant Dermatologist who specialises in skin cancer diagnosis and management and will be able to advise you regarding the benefits of skin cancer surveillance.
During an appointment, you can opt to have a full skin check using Dermoscopy which produces views of individual lesions in high magnification. This requires training to analysis specific features which might suggest early changes of skin cancer. Where necessary, you can opt to have professional medical photos taken of your skin to use as a guide for monitoring your skin and looking for changes in your moles.


The following ABCDE assessment may help your assess your moles to determine if you have be reviewed by a specialist.

Imagine dividing your mole into two. One side should mirror the other side. If it does not, this could be a concerning change.

Look at the border of your moles. This is normally smooth all the way round. A jagged or moth eaten border may be a concern.

Moles are usually a single colour throughout. If there is more than one colour, particularly with asymmetry, ask for your mole to be reviewed by a specialist.
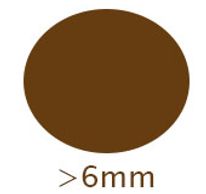
Whilst moles can be any size, small moles are less concerning. Moles beginning than 6mm may need a review particular if the size has changed over time.

Has your mole changed over time? A change in a mole may warrant review by a specialist.
Melanoma is a type of skin cancer which affects pigment cells called melanocytes. They therefore tend to be brown in colour.
It is usually recognised by a change in a mole or a new mole developing which you have not had previously,
One way to assess a mole for skin cancer is to the ABCDE criteria in the section above. If you have concern that your mole fits any of these criteria, consider seeing a skin specialist for a review with Dermoscopy. If there is concern following this, you may be advised to have the mole removed to send for analysis under the microscope. For further information on this type of procedure, see excision in the minor procedures section.
The British Association of Dermatology is a useful resource for information on Melanoma.
Please click below for further information.
If your mole has any concerning features, you may be advised to have it removed for analysis under the microscope.
If this is confirmed to be melanoma, you will be advised to have a further "wide local excision" around the initial scar. This adds a safety margin to ensure the melanoma is fully removed and reduces the chance of it coming back in the future. The size of this safety margin is dependent on the thickness of melanoma, known as Breslow thickness. You may also be advised to have a Sentinel Lymph Node Biopsy where a dye is injected into the initial scar site. The close draining lymph gland can then be identified and removed at the same time. This gland will be assessed under the microscope to see if there is any sign of early spread of the melanoma. If positive, you may be offered further treatment such as immunotherapy to target the melanoma.
Following this second procedure, you will start attending regular follow up to monitor for any recurrence. During this time, the specialist will check your lymph glands to ensure they are not swollen which may be a sign of the cancer spreading.
The typically follow up routine is 3 monthly for the first 3 years and then 6 monthly for another two years.
You will also be educated on how to feel your own lymph glands between appointments. Melanoma UK have produced a useful video to guide you on feeling your lymph glands. This can be accessed by clicking here.

This website uses cookies. By continuing to use this site, you accept our use of cookies. Privacy Policy